I recieved a lovely email from a reader this week who wanted me to write up a little something on a “Day in the Life of an RD”…so, I did! I get a lot of emails about people pursuing a career in dietetics, or a career change to dietetics, and various questions about the educational and career paths for dietitians…and I am always happy to help! I am passionate about what I do and truly, whole-heartedly LOVE my work. It’s not work if you love what you do, right? 😉
As a little background, I work as a dietitian in an out-patient clinic in a rural community outside of Tulsa. For patient safety and to remain compliant with HIPPA laws, I cannot disclose identifiable information on patients or my place of work. We do have several physicians on staff as well as 8 nurses, 4 pharmacists and pharmacy technicians, 2 dietitians, ultrasound technician, radiology technician, physiologists, ophthalmologists and optometrists, phlebotomists (and a laboratory), as well as per diem podiatrists, endocrinologists, pediatricians, etc. Basically, we are one-stop shop for health care and accept all major medical coverage and insurance.
I work Monday through Thursday, 7am to 5:30pm and for the most part schedule my own patients. If a referral is made for the dietitian, a receptionist books a patient in for a 1-hour appointment. I see primarily diabetic and bariatric patients, as well as those needing diet assistance to manage other conditions such as hyperlipidemia, hypertension, anemia, non-alcoholic fatty liver, metabolic syndrome, gout, renal insufficiency, pre-natal nutrition, and digestive health (i.e. Crohn’s, Celiac disease, etc.). But it is fair to say 80% or more of my time is spent on diabetes and bariatrics. I work on 30-minute slots and bill for medical nutrition therapy in 15-minute increments.
Let me set the scene…
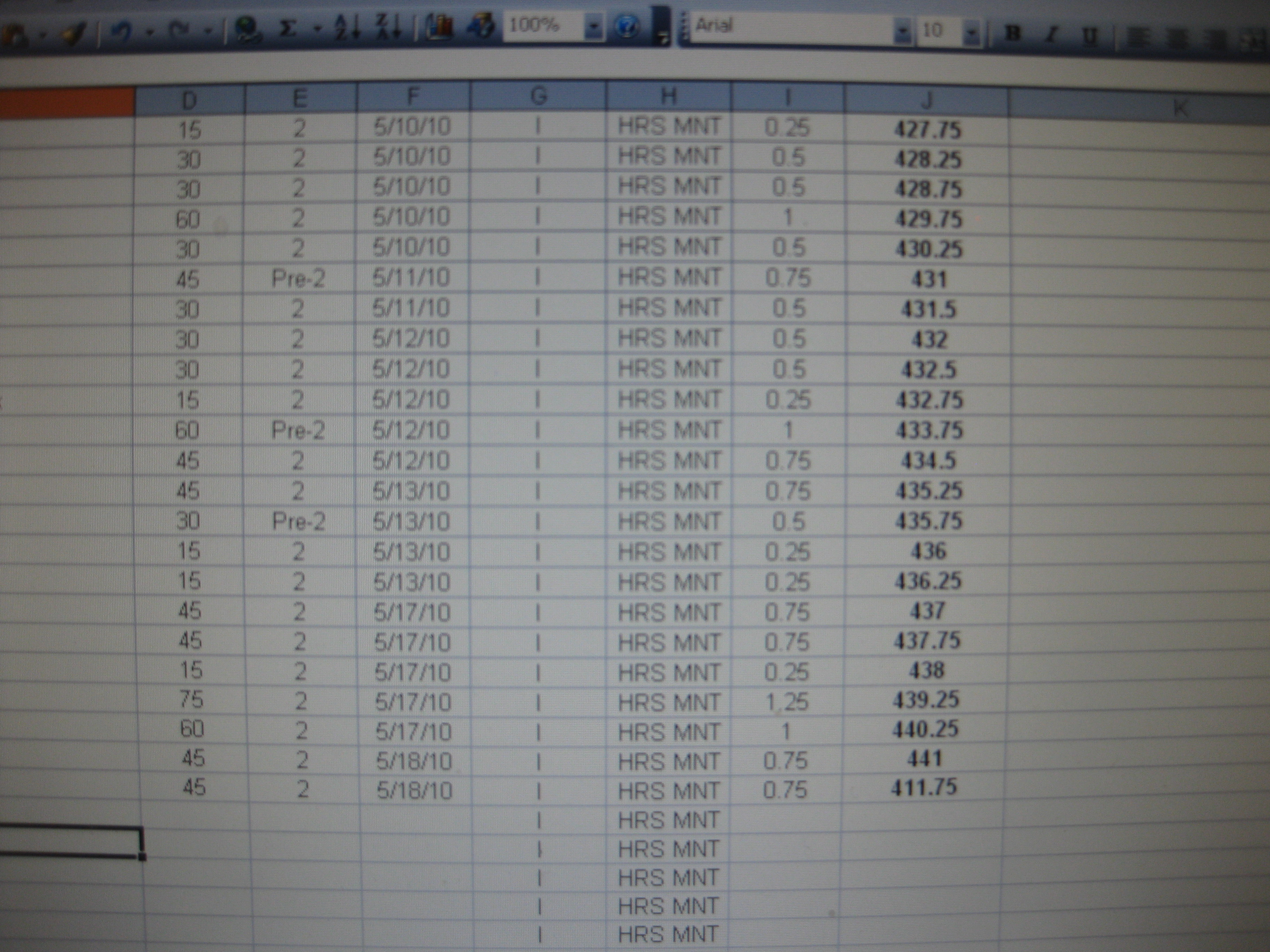
Currently, I am pursuing the Certified Diabetes Educator (CDE) credential. I currently have 445 hours and need 1,000 to sit for the exam. Logging my hours:
This is (part of) the form RD’s use to chart in my clinic. We are making the switch the Electronic Health Records (EHR) in the coming months.
Here is how insulin pens work:
[youtube=http://www.youtube.com/watch?v=Xz4lWM6vtf0]
Breakfast at my desk:
My work station:
Lunch at my desk:
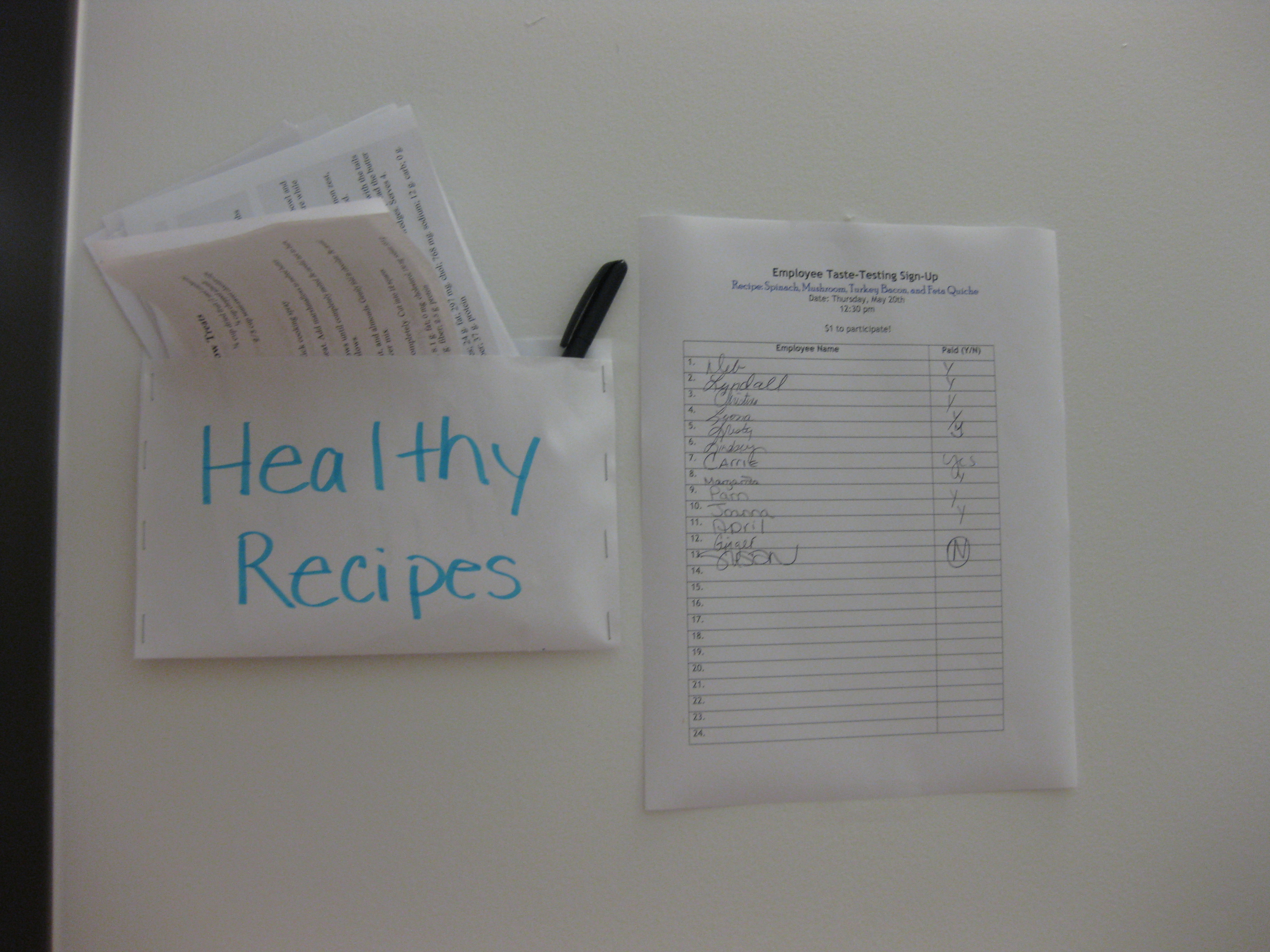
Employee Taste Test Sign-Up!
Tuesday went something like this…
7-8am: Check my schedule (no 7:30am appointment – woo!), catch up on emails, eat breakfast at my desk, and finish any charting left from the previous day
8am: New onset type 2 diabetic wanting to control blood glucose through diet and exercise. Full diabetes diet and glucometer education completed. Discussed the role of oral agents to help control diabetes (45 minutes)
9am: Weight management follow-up – patient is trying to lose 40 lbs for her 50th birthday in 5 months – down 9 lbs in 3 months so far (60 minutes)
10:30am: Uncontrolled diabetic on insulin – discussed recommitting after “falling off the wagon” (45 minutes)
11:20am: Uncontrolled type 1 diabetic following up regarding carbohydrate to insulin ratio. Food journals and insulin regimens reviewed, glucometer downloaded to analyze. Recommended no changes in insulin dosing as fasting and post-prandial blood glucose goals were being met (45 minutes)
12:30pm: Surprise appointment! I went out to my car to get my water bottle and a patient asked me in the street to download his glucometer and give him more testing strips. The patient is a controlled type 2 diabetic who I have worked closely with over the course of 9 months to get his blood glucose levels within normal limits. He now journals all of his intake and checks his blood glucose up to 6x a day (45 minutes)
1:15pm: QUICK 5 minute lunch at my desk
1:20pm: Weight management follow-up. Patient lost 4.3 lbs in 2 weeks on a 1,800 calorie diet. Patient is considering bariatric surgery through our clinic (30 minutes)
2pm: Weight management follow-up. Patient lost 3.5 lbs in 2 weeks. Young, disruptive child present at session. Patient goals include meal planning and making food stamps last longer throughout the month (45 minutes)
2:45pm: Patient was rescheduled – he did not bring his glucometer or food journals/pattern management to meeting and therefore no insulin adjustments could be made.
3pm: Follow-up with uncontrolled type 2 diabetic on insulin and strict pattern management. Called patient’s physician and recommended a change in Levemir (long-acting insulin) – verbal order given over the phone (30 minutes)
3:45pm: Follow-up weight management and uncontrolled hypertension; 0.8 lb weight gain in 2 weeks. Patient was seeking advice on diet pills and how to manage “dieting” with unsupportive friends, co-workers, and husband (45 minutes)
4:30pm: Weight management follow-up – I have been seeing this patient for 9 months without significant weight loss, yet she attends all of our appointments and wants to continue coming to RD meetings (30 minutes)
5-5:30pm: Catch-up on charting, returns urgent emails and phone calls, and head home!
WHEW!
There were 14 appointments scheduled on this day – 2 called to cancel, 2 no-showed, and I had 1 walk-in patient.
Likes and Dislikes
I love the critical thinking and intense patient-provider interaction involved in diabetes care. Plus, I do have some of the best patients :). And most of you know I am passionate about diabetes, I love working in diabetes. I hate the early hours…mornings are rough…and the fact that most blogs are blocked at work 🙁 And…I can always want more money, right? 😉
There you have it…a Day in the Life of an RD!
Question: What is your current profession? What do you love and hate most about YOUR current role?
Work hard 😉 ,







Thanks so much for a great post! It sounds like a busy day but one that keeps you on your toes.
I’m a language teacher. I love watching students progress throughout the year, building their language skills. I (sort of) dislike grading; however, that said, I recognize the importance of a good and balanced assessment program. Everyone, myself included, needs to know how they’re doing’! Have a great Thursday!
I love how much interaction you have with people throughout the day — it must make your job so interesting and fulfilling. And I can imagine how wonderful it is to see people getting results and living happier lives because of what you do!
I’m pretty sure that if I weren’t doing this whole doctor/MD/PhD business then I would have loved to become an RD. Nutrition is possibly my favorite thing to talk about! I love that you love your job 😛
cool post Nicole. Let me pitch in how my day looks like!
I have a son and wanted to spend more time at home with him, so I chose the consulting/project-based work. Dietetics is a very family-friendly profession. I work 2 days a week, and these days, I either spend a whole day working per diem as a clinical dietitian in an acute care hospital. When I’m not in the hospital, I’m working on a project designing power point presentations for a general audience as part of a contract–so I work from home or any coffee shop with wireless internet. If not these two, I’m trying to do freelance writing, so I may be writing queries or writing an article (when the query gets accepted) so every day is a whole new day! Other days, I’m working on my master classes 🙂
I love the versatility, the broad range of activities, and the flexibility. I like doing my own thing. I love freelance writing but I hate the rejection I have to go through before one query gets accepted. The money is not consistent, so the only way I can do this is because my husband can take care of the bills and benefits, and I can make whatever I can extra. However, I know single dietitians who have this type of consulting work and are able to financially support themselves.
Wow, Nicole! That’s a long and very tightly packed day. Kudos to you. But like you said, as long as you love what you do, it’s not like going to work!
I love this – so interesting, never a dull moment it seems. I would be frustrated by the people who bring their disruptive children or the ones that don’t bring their food journal. How are you supposed to help them if they don’t provide resources?!
I work in Human Resources for a large retail developement company. We’re very busy doing all sorts of things – never a dull moment. I love my job, but sometimes i’d like more flexability like on a gorgeous 80 degree like today 🙂
I loved this post! It sounds like such a packed, but fun, day!
This sounds actually kind of fun! It must be really fulfilling to see your patients’ progress. 🙂 Thanks for sharing!
Love this post! I know you had already told me a bit about your work when we met, but it was cool to see your day hour by hour!
I’m a college instructor. I love my students (well, most of them). The biggest challenge right now are budget cuts, which directly affect our teaching…
Great post! I love that it sounds like you keep busy and the day flies by…..and then you get to leave at 5:30. Granted, I don’t start until 9/9:30 some days, but sometimes I would love to have a consistent job where I could leave on time every day (and I’m sure you have your late days too). But things I love about my job are that I can move to Singapore for 3 years when I’m only 28, I can work independently and be a little bit of my own boss; and while sometimes the schedule is demanding, it can also be pretty flexible like this morning when I had to work from home.
Love this post!! This is great for readers to see!
Loved hearing about your day. It is packed! I would be exhausted!
I loved reading about your day. It’s always interesting how other people spend the 9 to 5. I’m a writer so my day is spent at the computer. I love to write, but days like today—when I have a pounding headache—I wish I could do something that didn’t involve staring at the computer!
This is a great post! Seriously, when I was thinking about becoming an RD I googled all over the place for what a “day in the life” was like and came up with pretty much nothing. I thought this was really interesting! It makes me think I should do a “day in a life” post about what it was like being a diet tech (which I’m not anymore, but maybe other people will like to know).
Thanks for this post! It was very informative and gave a good picture of what you do.
Nicole, I LOVED reading this! You are definitely a BUSY girl, for sure. I often wonder the play-by-play of people’s jobs. I can tell you love your job, and it just seems so rare (TOO rare) to find that these days. I know it sounds cheesy, but I know I’m meant to be in a field where I am helping people, too. It has to make you feel SO good to know you’re making a difference in these people lives – and acting quite like a therapist would, too, I am sure!
My current profession = paralegal. Not too much I like about it – not to be negative, it’s just too rote and dry for me. 🙂 But that will change soon, God willing!
I’m not an RD, but I am a lifestyle and weight management consultant… I don’t ‘prescribe’ nutrition, but I do meet with people like you do to help them change their unhealthy habits and eat more nutritiously (is that a word? :))
I understand the days that are fun and rewarding- when people make progress! And the days that are frustrating… people not sticking to their commitments and always blaming something else… but overall, so rewarding! 🙂
Thanks for sharing this! It is so interesting, and I think that working with diabetes must be incredible, being able to help and encourage people to get better 🙂
Sounds like a busy day!
Similarly, my daily schedule is different – which is one thing I really like about my job. I hate doing the same thing day in and day out…!
Hi! I am also a dietitian! I work for WIC. It’s not my passion. NUTRITION is, but the WIC department is not. I started off as a clinical dietitian at the Univ. of Mich. Hospitals and had to switch to WIC when I moved in with my current hubby (for lack of other openings). I hope to someday have my own nutrition counseling business.
I love in this postion: the pay/benefits (not the reason to be at a job) I hate about this position: I don’t get to educate people the way I would like. I feel unfulfilled. That’s why I started my own blog, so I could write about things I wanted to and at least feel like I am informing someone!! Sorry for the rant!!
take care!
This is so interesting!!! I loved this post! So much goes into your work…I really admire people in this field.
Nice to know your life as an RD…lovely post
Very cool post–I find it very interesting, probably because I secretly want to be an RD or a zoo nutritionist. But ag teaching will do for now =). I must admit, I am a tad jealous of your work schedule! What I love about my job: working with kids, working outdoors with plants and livestock. What I don’t like: working erratic hours (as the FFA advisor), working a lot of weekends and my summer is not off at all.
Yep, sounds and looks about right. I did both outpatient and in patient and even alternated days. My current job is online teaching and then I tutor at the middle and high school so my schedule is different everyday and very flexible. I cram the gym in during the 11-12 time range and I usually eat lunch at home. Living overseas is very different, but when in the States, my day was, well, like yours! 🙂
Whew that is a busy day! I could see getting stressed at times working like that. But your work is so rewarding it makes it worth it. Loved reading your day.
i love this! thanks for sharing……to me it sounds like a long day….i am a teacher so i only usually work until 4…..
Great recap of you day. It’s so interesting.
I work in an industrial setting.
The best part of my work is when challenges come up or creative marketing is called for. I love to be busy.
Sounds like a crazy busy and challengin (in a good way!) day. My day job is in HR… Sitting all day. But my new addition of teaching bootcamp has been so wonderful and fun! I look forward to it so much. I love challenging the group past what they think they can do.
Wow, busy busy!! 🙂 Thanks for posting all this, Ive always wondered what it would be like.
Right now Im working as a receptionist at an office where I am the only girl. What do I like about it? That it makes me want to go back to school.
Lved that post! You’re a busy girl but you’re so passionate about your job, that’s fantastic!
Very interesting!! I loved getting a peek into your day!! 🙂
This sounds like a busy but really fun day Nicole! This job sounds perfect. And 4-ten hour days are awesome 🙂
Thanks for giving us a little peak into your daily life! My husband and I will be moving shortly (not sure where yet) and I really want to go back to become an RD. Am I on the older end to be pursuing a Master’s but better late then never, right? I am finished with my current corporate job in t-minus five days!
Interesting.
I’m sort of a graphic designer. I like being creative, but a lot of the time my job is slow and boring.
I loved this post! It seemed like a loooong day but you are doing something that you love so I am sure it makes it more tolerable…I can’t wait to do what I love to do!
great post and really highlights how important RD’s are and how hard we work
love ya
Oh! Nicole, your day is sure very busy…I am into science, therefore lots and lots of challenge 🙂
wat a cool day i want my life be like you but i am always free , in home enjoying holidays
I really like this post; I think it’s so interesting what other people do and breaking a day down into hour-by-hour accomplishments is a great way to learn about it
I love this so much; wish I could spend a day in your office shadowing you! I hope you enjoy work
Very interesting! I have to say that I have always wanted to work in an out-patient setting, as apposed to in-patient. I am not a clinical dietitian at heart, but if I had to, I would do out-patient. In fact, the VA out-patient rotation during my internship was one of my favorite rotations, I LOVED IT!
Wow! I loved this post! Very insightful and interesting 🙂
Sounds like a busy, but fun day! Are you by any chance attending the Healthy Living Summit!!
Loved hearing about your day! And I hear ya–I hate when blogs and other fun sites are blocked from work! I get it though … Anywho, great post and come 2 weeks from today, I’ll be joining the RD crew! FINALLY!
This is so interesting, Nicole! I’m glad to know you enjoy the work, even if the hours are early and long. I can imagine that you see ALL kinds of patients, including ones that are difficult to deal with or who are stubbornly noncompliant. Or who are a breeze to get along with and appreciate your help 🙂
I’m a dietetics student, but I do work for a private practice dietitian who also teaches at a college, works in Food Service, and counsels at other organizations. Dislikes: I HATE food service, but that’s what she does the most. Likes: Variety, feeling like I’m doing something positive 🙂
Self-employed in distribution. Love being my own boss but hate vehicles breaking down all the time!
Very nice post! I have a soft spot in my heart for Oklahoma, because I did an internship rotation in Norman, OK.
I’m a Registered Dietitian in Western Canada and I work in a community setting up north. I was very impressed by the very low number of ‘no-shows’ Prevention RD had that day. When I’m wearing my ‘outpatient’ hat, I’m lucky if 10% of my clients show up. Very frustrating.
That being said, I love the autonomy I have in my current position and that I get to be creative in planning my nutrition programming. I love being able to build relationships with individuals and my communities. My current position is so rewarding.
wow! interesting! very rare dietician wants to share a story to people about their business! as a dietician wannabe, i love all things about dietitian. hope i can be a success dietitian one day!
Hi there,
This is a great post for what I am going to school for! Going for my bachelors to become a RD and this is amazing to read. I’ve been trying to find ways to help people with nutrition and even myself since being diagnosed with PCOS at 16 years old.
Thank you so much!
Author
Hi Kiaya! Congratulations and choosing a very rewarding career! Love working as an RD! Best wishes to you – thanks for reading 🙂
Author
Hi Kiaya! Congratulations and choosing a very rewarding career! Love working as an RD! Best wishes to you – thanks for reading 🙂